Alaska Stands Alone as Medicare Advantage Plans Evade the Last Frontier

While more than half of American seniors have transitioned from original Medicare to the perceived advantages of private Medicare Advantage (MA) plans, Alaska remains a stark anomaly in the national healthcare landscape. By 2026, it will be the sole U.S. state where individual Medicare Advantage plans are entirely unavailable for general enrollment. This unique situation is not dictated by state legislation but is instead a consequence of a complex interplay between Alaska’s vast geography and its exceptionally high healthcare costs. Private insurers have found it economically unfeasible to establish the robust, low-cost provider networks that are the bedrock of the MA model in the Last Frontier.
Attempts to introduce individual MA plans in select Alaskan zip codes in 2022 and 2023 ultimately proved unsuccessful, with insurers withdrawing their offerings by 2024 due to insufficient enrollment and limited provider participation. This indicates a fundamental challenge in adapting the private insurance model to the realities of healthcare delivery in Alaska.
The Economic Realities Driving Alaska’s MA Absence
The fundamental reason for the absence of individual Medicare Advantage plans in Alaska lies in the economics of provider networks. Medicare Advantage plans operate by negotiating lower reimbursement rates with healthcare providers—doctors, hospitals, and specialists—to create a network that allows them to offer competitive premiums and benefits to enrollees. In Alaska, this model falters due to a confluence of factors that escalate healthcare costs and fragment service delivery.

Alaska’s healthcare system is characterized by its extreme geographical challenges. The sheer size of the state, coupled with its sparse population distribution and limited infrastructure, significantly increases the operational costs for healthcare providers. Transporting medical supplies, attracting and retaining medical professionals in remote areas, and the sheer distance patients must travel for specialized care all contribute to higher per-patient costs. Consequently, healthcare providers in Alaska are often hesitant to accept the lower reimbursement rates offered by private MA plans, which typically pay less than traditional Medicare.
Data from the Centers for Medicare & Medicaid Services (CMS) highlights this disparity. While national averages for Medicare Advantage reimbursement rates are set to balance insurer profitability with provider compensation, Alaskan providers often find these rates insufficient to cover their elevated operating expenses. According to KFF.org, Alaska has a higher-than-average rate of physicians opting out of the Medicare program altogether. In 2023, approximately 2.8% of physicians in Alaska declined to participate in Medicare, compared to a national average of less than 2%. This decision is directly linked to the financial viability of accepting Medicare-negotiated rates.
The economic strain on Alaska’s healthcare system is further underscored by its national ranking in per capita health spending. For the past 15 years, Alaska has consistently ranked among the top states for healthcare expenditure. In 2022, the state’s per capita health spending reached an estimated $13,642, placing it second only to Washington D.C. and significantly above the national average. This high cost of care directly impacts the profitability of private insurance plans, making it difficult for MA insurers to offer plans that are both financially attractive to them and beneficial to enrollees.
State economist Samuel Tappen, in a report for the Alaska Department of Labor and Workforce Development, has repeatedly pointed out that Alaska’s three largest urban centers—Anchorage, Juneau, and Fairbanks—have consistently held the top three positions for the highest urban health costs in the United States. This persistent trend reflects the pervasive nature of high healthcare expenses across the state, irrespective of location.

The Patient Experience: Navigating a Fragmented System
For Alaskan seniors, the absence of individual MA plans means their healthcare decisions are primarily guided by the framework of original Medicare, often supplemented by Medigap (Medicare Supplement Insurance) policies. While this offers a degree of freedom in choosing providers, it also presents its own set of challenges, particularly concerning access to specialized care.
Patients in Alaska frequently undertake long-distance travel to access specialized medical treatments. These journeys can span hundreds of miles, particularly for residents in rural areas who must travel to urban centers like Anchorage or Fairbanks for advanced medical services. This logistical hurdle not only complicates care coordination but also significantly inflates healthcare expenses, as patients incur costs for travel, accommodation, and lost time from work or personal activities.
The concentration of advanced medical services in a few urban hubs means that timely access to specialists can be a significant issue. While original Medicare provides broad coverage, the practical reality of securing appointments and receiving consistent care can be challenging for seniors who may face mobility issues or limited financial resources for extensive travel.
Alaska’s Senior Health Profile: A Paradox of Activity and Access Challenges
Despite the significant challenges in healthcare access and the absence of Medicare Advantage plans, Alaska’s senior population exhibits a surprisingly robust health profile in certain areas. The 2025 Senior Report from America’s Health Rankings places Alaska at a respectable 23rd overall for senior health. This ranking highlights a paradox: while the state faces significant hurdles in clinical care access, its seniors demonstrate high levels of physical activity and a generally positive self-reported health status.
Approximately 30.8% of Alaskan seniors engage in regular physical activity, a figure that surpasses the national average. Furthermore, their rate of inactivity (29.2%) is lower than the national average of 31.7%. This active lifestyle contributes to better overall health outcomes and potentially mitigates the impact of chronic diseases.
More strikingly, 43.4% of Alaskan seniors report their health status as "Excellent" or "Very Good," a rate that outperforms the national average of 40.5%. This suggests that factors beyond the specific structure of Medicare plans, such as lifestyle, environment, and personal resilience, play a crucial role in the well-being of the state’s older population.
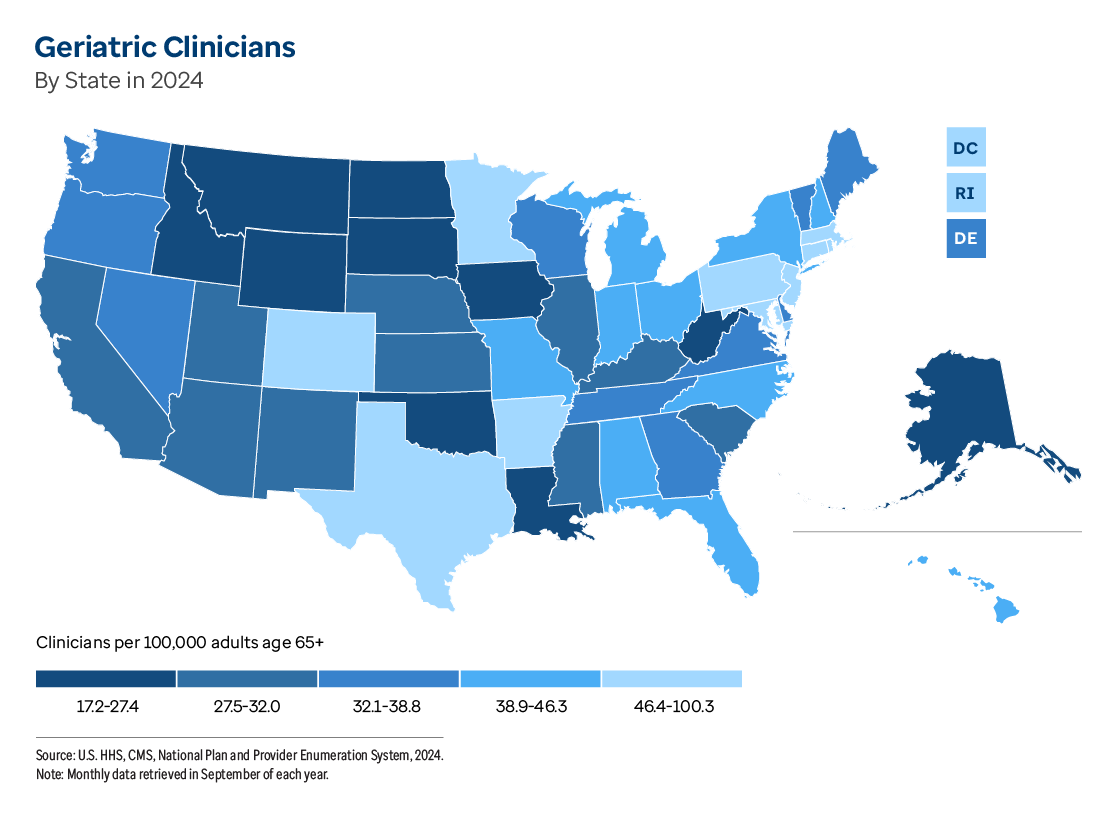
However, the report also starkly identifies Alaska’s primary weakness: clinical care access. The state ranks alarmingly low at 42nd for the availability of geriatric clinicians per 100,000 seniors, with only 24.7 geriatric clinicians available compared to the U.S. average of 39.9. This shortage is a critical barrier to comprehensive geriatric care, impacting the ability to manage complex health needs effectively.
The rate of "avoidable deaths" among seniors in Alaska, defined as deaths occurring between the ages of 65 and 74 that could potentially be prevented with timely and effective healthcare, is reported as moderate. Encouragingly, early deaths in this age group have seen a notable decrease of 15% since 2021, suggesting that chronic disease management efforts, even within the existing healthcare framework, are yielding positive results.

Who Are the Few Alaskans Enrolled in MA Plans?
While individual enrollment in Medicare Advantage plans is not an option for most Alaskans, approximately 2% of the state’s Medicare beneficiaries are enrolled. These individuals fall into two distinct categories:
-
Dual-Eligible Beneficiaries: This group comprises individuals who are eligible for both Medicare and Medicaid. These beneficiaries often have specific needs and may be enrolled in MA plans designed to coordinate benefits between the two programs, particularly Special Needs Plans (SNPs) that cater to individuals with chronic conditions or specific healthcare needs. These plans are often sponsored by health systems or provider groups that have established contracts with the state’s Medicaid program.
-
Institutionalized Individuals: Seniors residing in long-term care facilities, such as nursing homes, may be enrolled in MA plans that have specific contractual agreements with these institutions. These plans are designed to manage the complex and ongoing care requirements of residents in such settings.
In both these cases, the enrollment is typically not a choice made through the standard Medicare Marketplace but rather a consequence of specific eligibility criteria or contractual arrangements between providers and insurers catering to particular demographic or institutional needs.
The Pros and Cons of Alaska’s Unique Medicare Landscape
The absence of individual Medicare Advantage plans in Alaska presents a unique set of advantages and disadvantages for its senior population:
Pros:
- Unrestricted Provider Choice: Seniors enrolled in original Medicare and Medigap have the freedom to choose any doctor or hospital that accepts Medicare, without being restricted by network limitations. This is particularly beneficial in a geographically vast state where provider availability can be scarce.
- Predictable Costs (with Medigap): While original Medicare has deductibles and coinsurance, Medigap plans standardize these costs, offering a predictable out-of-pocket expense for covered services. This can be advantageous for seniors who prefer financial certainty over potentially lower premiums with MA plans that may have higher out-of-pocket maximums for certain services.
- No Surprise Network Changes: Unlike MA plans, which can change their provider networks annually, original Medicare ensures that a provider’s participation in Medicare remains consistent, reducing the risk of a sudden change in where a senior can receive care.
Cons:
- Potentially Higher Out-of-Pocket Costs (without comprehensive Medigap): While original Medicare is broad, it does have deductibles and copayments. Without a robust Medigap plan, these costs can accumulate, especially for seniors with frequent healthcare needs.
- Absence of MA "Wellness" Programs: Many MA plans offer additional benefits not covered by original Medicare, such as routine dental, vision, and hearing care, as well as fitness programs and transportation assistance. Alaskan seniors relying solely on original Medicare miss out on these supplemental perks.
- Limited Navigation and Care Coordination: MA plans often provide integrated care coordination services, helping members navigate their healthcare journey and manage chronic conditions. Seniors on original Medicare may need to actively manage this coordination themselves, which can be challenging given the state’s healthcare access issues.
- Higher Premiums for Medigap: Medigap plans, particularly those offering comprehensive coverage, can be expensive. For seniors who might have qualified for low-premium MA plans in other states, the combined cost of original Medicare premiums and a Medigap policy can be substantial.
Looking Ahead: The Future of Healthcare in Alaska
Alaska’s unique position in the Medicare landscape underscores the challenges of delivering affordable and accessible healthcare in sparsely populated, geographically challenging regions. The state’s commitment to maintaining a system that prioritizes unrestricted provider choice for its seniors, even without the widespread adoption of Medicare Advantage, reflects a distinct approach to elder care.

As the nation continues to grapple with rising healthcare costs and evolving insurance models, Alaska serves as a critical case study. The state’s efforts to address its healthcare workforce shortage and improve infrastructure are crucial for ensuring that its active and resilient senior population can continue to receive the care they need, regardless of the insurance plans available. The success of initiatives aimed at expanding telehealth services, supporting rural health clinics, and incentivizing medical professionals to practice in the state will be pivotal in shaping the future of senior healthcare in the Last Frontier. Ultimately, Alaskan seniors demonstrate that a focus on active living and direct provider access can lead to positive health outcomes, even in the absence of the widely adopted Medicare Advantage model.








