Transforming Healthcare: How Conversational AI is Redefining Patient Engagement and Operational Efficiency
The healthcare industry stands at a critical juncture, grappling with an unprecedented confluence of rising patient demand, persistent staffing shortages, and an ever-present labyrinth of compliance risks. Simultaneously, there is an intensifying expectation for healthcare providers to deliver faster access, achieve superior patient outcomes, and reduce costs, all while meticulously safeguarding protected health information (PHI) across every interaction. In response to these complex pressures, healthcare organizations are increasingly turning to sophisticated conversational Artificial Intelligence (AI) technology as a transformative solution, modernizing everything from call handling and messaging to comprehensive digital engagement strategies. By embedding AI directly into their communication platforms, providers can significantly accelerate access to care, automate routine administrative tasks, and alleviate the immense strain on staff, crucially, without needing to expand their workforce. This strategic integration is not merely about technological adoption; it represents a fundamental shift in how healthcare systems interact with patients and manage their internal operations, promising measurable value and a more resilient future.
Understanding Conversational AI in the Healthcare Ecosystem
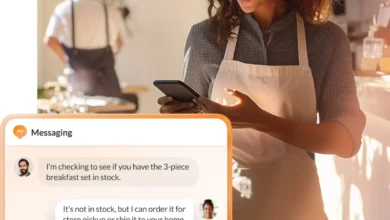
Conversational AI for healthcare is an advanced technological paradigm that empowers both patients and staff to interact with digital systems using natural language, much like conversing with another human. Unlike rudimentary AI chatbots that typically address simple frequently asked questions (FAQs) through predefined scripts, conversational AI is engineered to comprehend intent, execute complex actions, and seamlessly integrate with vital clinical and business systems. This capability allows it to manage entire workflows, such as a patient calling after hours to effortlessly reschedule an appointment, or using a web chat to resolve billing queries, or confirming upcoming appointments via SMS—all powered by real-time data retrieved from electronic health records (EHR) and scheduling platforms. The distinction is crucial: while a chatbot might offer static information, conversational AI facilitates dynamic, goal-oriented interactions that drive tangible outcomes.
The urgency for such technologies has never been greater. Patient expectations have undergone a fundamental transformation, shaped by their experiences with other industries. Individuals now anticipate the same speed, intuitiveness, and personalized service from their healthcare providers as they receive from their banks, favorite retailers, or when booking travel. Whether checking lab results, settling a bill, or arranging follow-up care, the bar for digital convenience and efficiency is exceptionally high. The gap between these evolving expectations and the traditional healthcare experience has significant consequences. Data from McKinsey indicates that limited access to care and difficulties in securing appointments with preferred practitioners are among the primary reasons U.S. patients opt to switch providers. Studies further reveal that a substantial 60% of surveyed consumers report encountering hurdles when attempting to schedule appointments. Compounding this challenge are persistent staffing shortages, widespread clinician burnout, and tightening budgetary constraints, making the traditional solution of increasing headcount increasingly unrealistic. Conversational AI platforms thus offer a pragmatic and scalable path forward, handling routine interactions, intelligently directing complex requests to appropriate personnel, and providing staff with real-time support, thereby enabling them to concentrate on higher-value clinical and patient-facing work. Early adopters, such as healthcare organizations utilizing RingCentral’s AI tools, have reported a notable 42% increase in patient satisfaction and a 53% surge in employee satisfaction, underscoring the dual benefits of this technology.
The Mechanics of Healthcare Conversational AI
At its core, conversational AI operates on a straightforward yet powerful logic: comprehend the user’s request, determine the most appropriate next step, and then either execute the action directly or route the interaction to the relevant human agent. In a voice-first, enterprise-grade platform, this unfolds through several sophisticated layers. Firstly, advanced Natural Language Processing (NLP) interprets the nuances of human speech or text, understanding context, sentiment, and intent far beyond simple keyword matching. This allows the system to engage in adaptive conversations that mimic human interaction, rather than following rigid, predefined scripts characteristic of traditional Interactive Voice Response (IVR) systems. Secondly, sophisticated machine learning algorithms enable the AI to continuously learn and improve from each interaction, refining its understanding and response accuracy over time. Thirdly, seamless integration capabilities allow the AI to tap into a vast network of existing healthcare systems—EHRs, scheduling platforms, billing systems, and CRM tools—in real-time. This ensures that the AI’s responses and actions are always informed by the most current and accurate patient data.
However, the efficacy of conversational AI in a healthcare setting extends beyond the technology itself. Critical factors such as voice quality, system reliability, the depth of integration with existing infrastructure, and enterprise-grade security protocols are paramount. These elements collectively determine whether the AI solution truly delivers on its promise of efficiency and improved patient experience while adhering to stringent compliance guardrails, particularly concerning the privacy and security of PHI.
Tangible Benefits: Transforming Operations and Outcomes
The adoption of conversational AI tools in healthcare is driven by a clear strategic imperative: to enhance patient access, elevate the patient experience, and optimize operational efficiency. Organizations implementing these solutions consistently report measurable impact across several key areas.
-
Reduced Call Abandonment and Expedited Access to Care: Conversational AI effectively offloads routine requests, eliminating the need for patients to wait in lengthy queues for simple tasks. This significantly shortens wait times, reduces call abandonment rates, and frees up human staff to focus on more clinically important or complex conversations. The net result is faster, more equitable access to care without the burden of increasing headcount. This directly addresses one of the major pain points for patients and a significant operational inefficiency for providers.
-
Increased Patient Satisfaction and Retention: In today’s competitive healthcare landscape, ease of access is a primary determinant of patient loyalty. Conversational AI provides 24/7, multilingual, omnichannel access across phone, SMS, and digital platforms. When interactions are consistent, predictable, and efficient, patients develop greater trust in their provider, leading to increased adherence to care plans and higher retention rates. A survey by Tebra highlighted that 30% of providers identified outdated technology as a regular barrier to scheduling, with 61% believing AI would improve these processes. Furthermore, Phreesia’s insights reveal that 18% of patients now prefer online scheduling methods over traditional phone or in-person interactions, underscoring the demand for diverse and easy-to-use channels.
-
Cost Control and Quality Maintenance: Automation is a powerful lever for shifting repetitive, low-risk tasks from human staff to AI. This means teams spend less time on activities like resetting passwords or confirming appointments and more time resolving complex billing issues or clinical concerns that require human empathy and expertise. This strategic reallocation of resources enables healthcare organizations to manage growing patient volumes without proportional increases in labor costs, thereby protecting margins while maintaining or even enhancing service quality.
-
Improved Staff Productivity and Reduced Burnout: High interaction volumes, frequent interruptions, and constant context switching are major contributors to healthcare staff burnout. Conversational AI mitigates these issues by streamlining workflows and providing relevant, real-time information. For instance, AI can summarize prior patient interactions and highlight key details, drastically reducing after-call work and improving consistency. This allows teams to spend less time toggling between disparate systems and more time delivering meaningful, personalized patient care, thereby enhancing job satisfaction and reducing turnover.

-
Strengthened Visibility, Consistency, and Compliance: A unified communication platform that incorporates conversational AI provides a comprehensive overview of demand patterns, patient intent trends, and service gaps. This centralized control enables organizations to standardize scripts, disclosures, and triage workflows, ensuring consistency and allowing for rapid updates as policies evolve. Crucially, every patient interaction is logged, creating a full, auditable record that supports robust compliance, continuous quality improvement initiatives, and robust governance frameworks, significantly reducing regulatory risk.
Key Applications: Where Conversational AI Delivers ROI
To achieve measurable return on investment (ROI), healthcare organizations should prioritize the deployment of conversational AI in high-volume, repeatable workflows. These areas consistently demonstrate strong returns.
-
Patient Engagement and Virtual Health Assistants: Virtual AI assistants offer 24/7, guided support without the need for additional staff. Instead of navigating cumbersome phone trees, patients can simply state their needs, and the AI will complete the task. High-impact applications include:
- Appointment Management: Scheduling, rescheduling, cancellations, and confirmations.
- Pre-registration and Onboarding: Guiding patients through necessary forms and information gathering before visits.
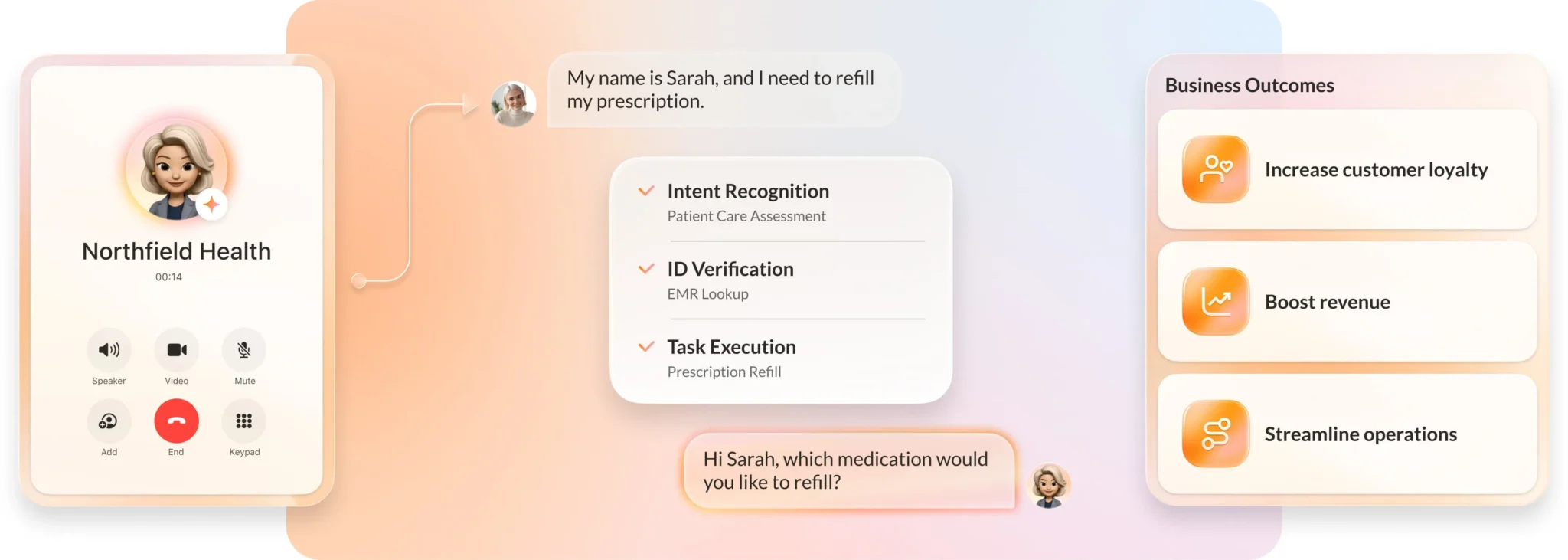
- Prescription Refills: Automating requests and checking status.
- Post-Visit Follow-ups: Reminders for medications, physical therapy, or subsequent appointments.
- General Information: Answering FAQs about clinic hours, services, and directions.
-
Administrative Automation and Cost Control: Administrative complexity is a significant driver of unnecessary costs in healthcare. Conversational AI reduces this burden by automating repetitive administrative tasks. Common starting points include:
- Billing Inquiries: Answering questions about statements, payment plans, and balances.
- Insurance Verification: Checking eligibility and benefits in real-time.
- Technical Support: Assisting with patient portal password resets or basic troubleshooting.
- Referral Management: Initiating or tracking referrals between specialists.
The AI can authenticate patients, retrieve real-time data, update records, and route calls intelligently without the need for rigid menu selections, dramatically improving efficiency.
-
Clinical Support and Real-Time Guidance: Conversational AI is designed to augment, not replace, clinical judgment. Healthcare organizations are leveraging AI to:
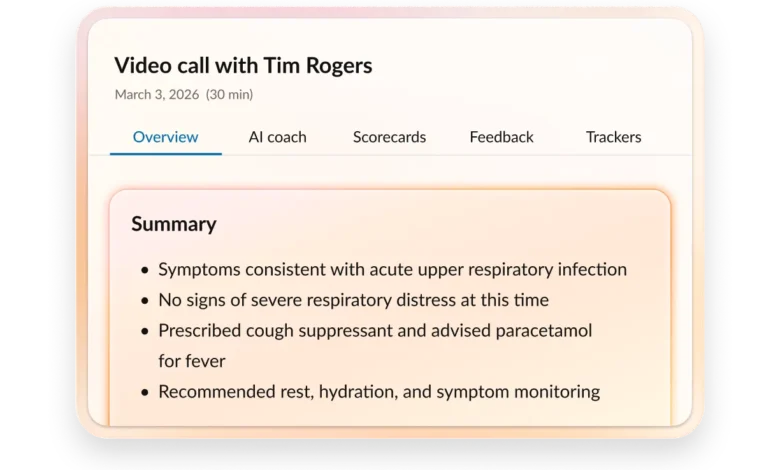
- Conduct Pre-assessments: Gathering preliminary patient information before a specialist consultation, enabling more efficient first visits.
- Assist with Care Coordination: Guiding patients through complex care pathways and providing information about different specialists or services.
- Provide Post-Discharge Instructions: Delivering clear, consistent instructions and reminders to patients recovering at home.
These tools reduce cognitive load and minimize context switching for healthcare professionals, ensuring they have access to the right information at the opportune moment. This leads to improved handoffs, more consistent patient care, and ultimately, better health outcomes. When deployed on a unified platform, intake, service, and follow-up converge into a single, cohesive workflow, providing unparalleled visibility and consistency across the entire patient journey.
Navigating Implementation: Challenges and Best Practices
Deploying conversational AI in healthcare is a complex undertaking, touching sensitive PHI, intricate clinical workflows, and core operational systems. Rushing the process or failing to secure organizational alignment can introduce operational risks rather than strategic advantages. Healthcare leaders must rigorously evaluate four critical areas.
-
Data Security and HIPAA Compliance: Protecting PHI is non-negotiable. The chosen platform must guarantee the security of patient information at every stage, from initial intake through follow-up. Essential requirements include end-to-end encryption for data in transit and at rest, robust access controls and authentication mechanisms, comprehensive audit trails, and, crucially, a Business Associate Agreement (BAA) that clearly outlines the vendor’s responsibilities under HIPAA. Full transparency into how the platform stores, processes, and secures patient data is paramount, and privacy and compliance leaders must be involved from the earliest stages of planning.
-
Integration Depth and Interoperability: The true power of conversational AI lies in its ability to interact seamlessly with existing healthcare systems. Prioritizing platforms that offer deep, real-time connectivity to EHRs, scheduling systems, and eligibility databases is vital. Without this, automation quickly falters. Key considerations include the availability of robust Application Programming Interfaces (APIs), adherence to interoperability standards like FHIR (Fast Healthcare Interoperability Resources), and proven success in integrating with a diverse range of vendor systems. Strong integration transforms AI from a mere front-end assistant into a powerful operational engine.
-
Robust Governance and Change Management: Effective governance is the bedrock for scaling conversational AI initiatives successfully. Organizations must clearly define the scope of AI deployment, the metrics for success, the roles and responsibilities of various stakeholders, and the processes for ongoing monitoring and optimization. Aligning IT, clinical, compliance, and operations leaders before launch is critical to prevent stalled pilot programs, the proliferation of "shadow IT" tools, and fragmented patient experiences. A well-articulated change management strategy is also essential to ensure staff adoption and address any anxieties about AI’s role.
-
Cultivating Patient Trust and User Experience: Automation must feel helpful and intuitive to patients, not confusing or impersonal. The AI should be designed to communicate clearly, offer appropriate empathy, and provide clear escalation paths to human agents when needed. A personalized approach, remembering past interactions, and maintaining context across channels are key to building trust. Poorly designed automation can rapidly erode patient trust and brand reputation, whereas well-orchestrated, user-centric AI interactions can significantly enhance satisfaction and reinforce a provider’s commitment to patient-centered care.
The Horizon: Future Trends Shaping Healthcare AI
Conversational AI is a rapidly evolving field, and healthcare organizations must select platforms that are future-proofed, supporting emerging trends rather than just current capabilities.
-
Proactive Patient Engagement: The paradigm is shifting from reactive support to proactive outreach. AI can trigger voice or messaging outreach based on appointment history, engagement patterns, or specific care team criteria. This includes automated post-discharge follow-ups, preventive screening reminders, or chronic care check-ins. This proactive approach helps close care gaps, reduce readmissions, and strengthen long-term patient relationships without increasing staff workload.
-
Seamless, Channel-Agnostic Experiences: Patients expect continuity. They might initiate contact via phone, switch to text, and follow up through a patient portal, anticipating that each interaction picks up precisely where the last left off, without the need to repeat information. Platforms built on unified voice, messaging, and video infrastructure are essential for maintaining shared context across all touchpoints, ensuring that AI capabilities extend consistently across every channel, rather than existing as a collection of disconnected tools.
-
Human-in-the-Loop and Augmented Intelligence: The ultimate goal is not complete automation, but rather to augment human capabilities. AI is increasingly designed to summarize interactions, suggest "next best actions" for agents, conduct pre-assessments for specialist care transitions, and flag high-risk patients in real-time. Healthcare professionals remain firmly in control, while AI handles the routine, data-intensive, or repetitive aspects of their work. The emergence of generative AI is beginning to influence how platforms draft responses and summarize documentation, though stringent healthcare governance requirements remain paramount for its widespread adoption.
-
Stronger Governance and Regulatory Oversight: As AI becomes more integrated into healthcare, regulatory frameworks are becoming more defined. Organizations will need platforms that provide transparent insights into AI decision-making processes, enforce robust governance controls, and can adapt quickly as standards evolve. Strong auditability, centralized policy management, and clear accountability mechanisms are no longer optional features but competitive necessities.
Strategic Directives for Healthcare Leaders
Conversational AI is a powerful operational capability, but to generate sustained ROI, it requires strategic focus, platform alignment, and robust governance from the outset.
-
Prove Value with Focused, High-Impact Workflows: Begin with areas where volume is high and the risk profile is low. Workflows such as appointment management, basic billing inquiries, and after-hours call handling are ideal candidates for pilot programs. Define clear success metrics upfront, such as self-service completion rates or cost per interaction, measure results early, and optimize quickly. This data-driven approach builds internal support and facilitates broader expansion.
-
Build on a Unified Platform, Not Point Solutions: Fragmented tools inevitably lead to fragmented patient and staff experiences. Select a platform that unifies communications, contact center functionality, and AI capabilities within a single, secure environment. Solutions that manage automated entry points, live-agent conversations, and internal collaboration on the same foundation reduce integration burdens, simplify governance, and provide end-to-end visibility across the entire patient journey.
-
Lead with Voice, Reliability, and Security: Healthcare operations still heavily rely on voice communication. If voice quality or system uptime falters, trust can erode rapidly among both patients and clinicians. Prioritize an AI-powered platform that offers carrier-grade voice quality, enterprise-level reliability with high uptime guarantees, and robust, HIPAA-compliant security measures baked into its core architecture.
-
Design AI to Augment, Not Replace, Your Teams: Automation should reduce workload and enhance human capabilities, not eliminate human judgment. Establish clear, intuitive escalation paths to agents and clinicians. Utilize AI tools to summarize interactions, surface relevant context, and reduce documentation burdens, enabling teams to dedicate more time to empathetic care. Ensure staff understands how AI integrates into their workflows and establish feedback loops for continuous refinement.
-
Establish Governance Before You Scale: Speed without governance introduces significant risk. Form a cross-functional governance group comprising IT, security, compliance, operations, and clinical leadership. Define clear policies for AI development, deployment, monitoring, and ongoing ethical considerations. This proactive approach ensures controlled growth and mitigates potential pitfalls.
-
Treat Deployment as an Ongoing Optimization Cycle: Conversational AI is not a static solution; it must evolve with the organization. Leverage analytics from the communications platform to identify new automation opportunities, refine existing workflows, and continuously improve performance over time. Regularly revisit the AI roadmap as regulations, patient expectations, and technological advancements shift.
A New Era of Intelligent Healthcare Delivery
Conversational AI represents a practical and powerful lever for improving access, enhancing efficiency, and elevating the patient experience—all without the need for increased headcount or incurring additional operational risks. For healthcare IT and CX leaders, the path forward is clear: strategically embrace this technology to empower staff, meet evolving patient demands, and build a more resilient and responsive healthcare system. The organizations that are pulling ahead are fundamentally rethinking patient needs and care delivery models, working smarter through intelligent automation. As patient expectations continue to rise and the pressures on healthcare teams remain relentless, modernizing patient communications with secure, AI-powered engagement at scale is no longer an option, but an imperative.